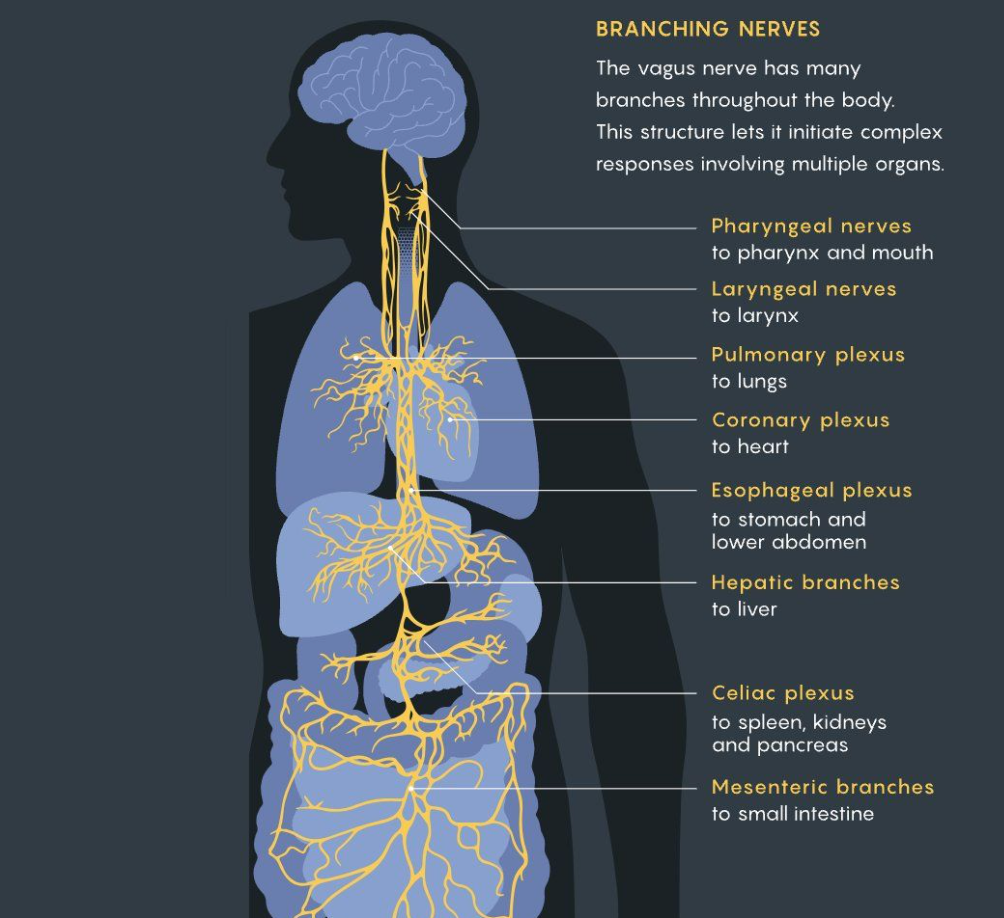
April 2026 Newsletter: The Vagus Nerve: Your Body’s Most Powerful Hidden Operator
My mission is to be the first woman in 4 generations to not develop Alzheimer’s Disease (AD). On my journey of discovering ways to mitigate my risk, I pass this information on to you in this Brain-Body-Health (BBH) Newsletter.
Hello, Brain Body Health Citizen Scientists
What Happens in Vegas…
This month I’m focused on a superpower that has profound effects on our brain and body — one that most people have never heard of, even though it’s been working quietly on their behalf every single moment of their lives. It’s called the vagus nerve. An old but new player in brain-body communication. Think of this nerve as the master operator of your central nervous system.
In case you missed it:
This newsletter is part of a series we have been doing on real-life superpowers.
January: Superpower of Awareness
February: Superpower of Genetics
March: Superpower of Play
I first encountered the vagus nerve in French medical school, where we spent hours drawing elaborate, colorful anatomical maps — tracing nerves through the body in their precise relationship to organs, muscles, and vessels. The vagus nerve was impossible to ignore. It wandered everywhere.
Later, during my psychiatry residency, vagus nerve stimulation was already being used to treat depression — long before we understood why it worked, long before we understood the inflammatory pathways that we now know this nerve so powerfully governs.
And then came Stephen Porges, and the discovery that changed everything about how we understand trauma. But we’ll get to that.
A Brief History of a Wandering Nerve
The name says it all. Vagus is Latin for “wandering” — and wander it does. The vagus nerve is the longest cranial nerve in the body, extending from the brainstem all the way down to the abdomen, touching the ears, heart, lungs, liver, pancreas, spleen, and most of the gastrointestinal tract along the way.
It has been studied since antiquity. The Roman physician Galen described it in the second century, calling it the pneumatikos — associating it with the spirit, the animating force connecting brain to body. He wasn’t wrong in spirit, even if the science has come a long way since.
The vagus nerve is the keystone of the parasympathetic nervous system — what we at BBH call the rest and digest system, the braking system to our cortisol-driven, sympathetic accelerator. It regulates heart rate, breathing, digestion, and immune function. All without you thinking about it for a single second.
I like to think of it as our telephone system. It makes communication possible between countries far and wide, between next-door neighbors, between the brain and the beating heart. There are actually two vagus nerves — one on each side of your neck — together made up of over 100,000 fibers, like a biological undersea cable. And what those fibers carry may be even more important than we ever imagined.
The Inflammation Connection: Your Body’s Hidden Fire
Here’s something that will change how you think about chronic disease. Inflammation isn’t just swelling after a sprained ankle — it’s a slow, systemic fire that burns quietly for years, and it sits at the root of more than 50 percent of deaths worldwide, including those from heart disease, stroke, cancer, diabetes, and Alzheimer’s.
The vagus nerve is your body’s built-in fire extinguisher.
Running through your neck like a cable, the vagus nerve carries what scientists call the cholinergic anti-inflammatory pathway — essentially, a direct line from your brain to your immune system. When activated, it signals your immune cells to stop releasing inflammatory proteins called cytokines. Think of it as the brain saying: “Enough. Stand down.”
When this pathway is strong and responsive, inflammation stays in check. When vagal tone is low — meaning the nerve isn’t communicating well — that regulatory signal weakens, and chronic inflammation can take hold. This is why researchers are now looking at small, pacemaker-like devices that stimulate this pathway to treat autoimmune conditions like Crohn’s disease and rheumatoid arthritis. The vagus nerve doesn’t just react to inflammation. It actively governs it.
Polyvagal Theory: When Safety Lives in the Nervous System
In the 1990s, neuroscientist Stephen Porges introduced a framework that quietly revolutionized how we understand trauma, connection, and survival. He called it Polyvagal Theory.
Porges discovered something the old textbooks missed: the vagus nerve isn’t one thing — it has two distinct branches, each with a very different job.
The older branch, the dorsal vagal system, is ancient. It’s the freeze response — the shutdown, the collapse you see in animals cornered by a predator, and in humans who have experienced overwhelming trauma. This is the nervous system’s last resort.
The newer branch — the one Porges identified — is the ventral vagal system. This is your social engagement system. It regulates your facial expressions, your tone of voice, your ability to listen and be truly heard. When it’s online, you feel safe. You can connect. You can think clearly. When it goes offline — when the body perceives threat — the higher functions drop away, and older survival circuits take over.
This is why trauma isn’t just a memory. It lives in the body, in the nervous system’s ongoing read of safety and danger. A trauma survivor isn’t “overreacting” — their ventral vagal system has learned, through experience, that the world is not safe. Healing, in this framework, isn’t only talk therapy. It’s teaching the nervous system — gently, repeatedly — that it’s safe to come back online.
The Dementia Connection: What This Means for Your Brain
Here’s where it gets personal — and urgent.
Population studies have found something striking: people who underwent vagotomy — surgical cutting of the vagus nerve, once done routinely for ulcers — showed a reduced risk of developing Parkinson’s disease and Alzheimer’s disease years later. At first glance, that seems backwards. But the answer points to the gut.
The vagus nerve is the main highway of the gut-brain axis, and emerging research suggests that the misfolded proteins associated with Parkinson’s and Alzheimer’s may actually travel up this highway — from the intestines to the brain. When the nerve was cut, that pathway was interrupted.
This doesn’t mean damaging your vagus nerve is protective — far from it. What it means is that what happens in your gut doesn’t stay in your gut. Chronic gut inflammation, poor microbiome health, and low vagal tone may all be early, silent contributors to neurodegeneration. Your brain health is being shaped, right now, by signals traveling up from your intestines.
The good news: vagal tone is something you can actively cultivate.
Toning Your Vagus: Small Habits, Profound Effects
You can’t see your vagus nerve. You can’t feel it the way you feel a sore muscle. But you can train it — and the evidence for how to do that is surprisingly accessible and low-tech.
Think of vagal tone the way you think of cardiovascular fitness. It’s not fixed. It responds to practice. And the practices that build it are things your grandmother probably already knew were good for you.
Breathe like you mean it. The fastest, most well-studied vagal intervention we have. The key is longer exhales than inhales. Try inhaling for 4 counts, exhaling for 6 to 8. That extended exhale activates your vagus nerve and measurably slows your heart rate within minutes. Five to ten minutes a day, over time, increases baseline vagal tone. This is not meditation as a concept. This is physiology.
Hum, sing, chant — out loud. The vagus nerve runs alongside the muscles of your larynx and pharynx. Vibration from humming or singing literally stimulates the nerve. This is why choral singing across cultures has always felt communal and calming — it’s not just psychological. Try humming in the shower, chanting, or gargling with water for 30 seconds. Sounds silly. Works anyway.
Cold water on your face. Splashing cold water on your face — or ending your shower cold — activates the diving reflex, an ancient vagal response that drops your heart rate and shifts your nervous system toward calm. Just 30 seconds of cold water on the face and back of the neck is enough.
Eat for your gut. Given everything we now know about the gut-brain axis, what you feed your microbiome matters. Fermented foods, fiber-rich vegetables, and polyphenol-rich foods like berries and olive oil all support gut diversity — which supports vagal signaling and reduces inflammatory load. Your dinner plate is a neurological decision.
Connect. Really connect. Feeling safe in the presence of another person is one of the most powerful regulators of the nervous system we have. Eye contact, attuned conversation, laughter, touch — these are direct inputs to your ventral vagal system. Loneliness, by contrast, is a chronic stressor that suppresses vagal tone and drives inflammation. Your social life is part of your brain health protocol.
Move your body — gently and regularly. Moderate aerobic exercise — walking, swimming, cycling — consistently improves heart rate variability, the best proxy measure we have for vagal tone. Slow, rhythmic movement done regularly is more beneficial than intense sporadic bursts.
What Happens in Vagus Doesn't Stay in Vagus
What happens in your gut travels to your brain. What happens in your immune system shapes your mood. What happens in your early life — the wounds, the losses, the moments of feeling truly unsafe — lives on in the tone of a nerve you’ve never seen and cannot name.
The vagus nerve is not a wellness trend. It is a 2,000-year-old anatomical reality we are only now beginning to understand in full. Low vagal tone quietly drives inflammation. Chronic inflammation quietly drives dementia, heart disease, and autoimmune illness. And the practices that restore vagal tone — breathing, singing, cold water, genuine connection, good food, gentle movement — are among the oldest, most human things we do.
You don’t need a device or a prescription to start.
You need a long exhale — and someone to share dinner with.
Resources:
StatPearls: Vagus Nerve Anatomy — ncbi.nlm.nih.gov/books/NBK537171
Li Ma et al., “The vagus nerve: An old but new player in brain-body communication,” Brain, Behavior, and Immunity, 2025
The Polyvagal Institute — polyvagalinstitute.org
Attention: Brain Body Health is now on Substack. You can download it on your mobile device or computer.
Creating each newsletter takes dedication and passion. Supporting this work ensures it can continue to inspire and educate.
Venmo: @bettyglacy
PayPal: @BettyLacy932
To optimal health and peace for all!
Subscribe to the email list for news and updates on Body-Brain Health
“If you want to go FAST, go alone. If you want to go FAR, go together."
- African proverb
To our optimized health!